What is Hidradenitis Suppurativa?
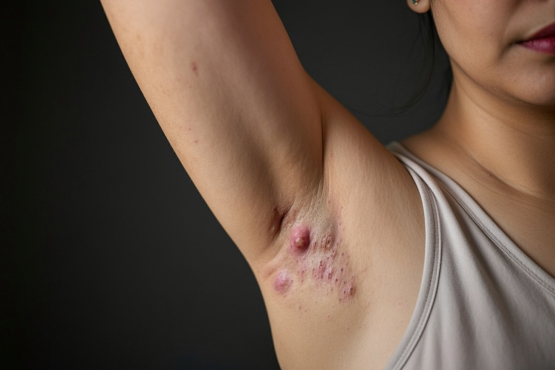
Hidradenitis suppurativa is a skin condition that causes small, painful bumps to form underneath the skin. These lumps can break open, and tunnels can form under the skin. This condition most commonly affects areas where the skin rubs together, such as the groin, buttocks, breasts, and armpits. Women, smokers, obese individuals, and African-Americans are disproportionately affected by the burden of this disease.
Symptoms of Hidradenitis Suppurativa
- Blackheads, often appearing in pairs
- Tunnels that form under the skin over time. These wounds are slow-healing and can leak pus or have an odor
- Scarring
- Painful bumps (nodules/abscesses) that appear in areas with hair follicles and oil and sweat glands, or areas where the skin rubs together
What Causes Hidradenitis Suppurativa?
Hidradenitis suppurativa (HS) may be triggered by an abnormal immune response or follicular occlusion, leading to the formation of painful nodules, abscesses, and sinus tracts under the skin. While the exact cause of HS is not fully understood, several risk factors are associated with the condition, including:
- Genetics: HS may run in families, suggesting a hereditary component.
- Hormones: Sex hormones play a role, which may explain why the condition often starts after puberty.
- Obesity and metabolic syndrome: These can worsen inflammation and are common among HS patients.
- Smoking: Strongly associated with moderate to severe hidradenitis suppurativa.
- Bacterial infection: Although not the cause, secondary infections may worsen the disease.
HS is sometimes associated with other conditions such as inflammatory bowel disease, acne conglobata, pilonidal sinus, and squamous cell carcinoma arising from chronic inflammation.
Who is a Good Candidate for Hidradenitis Suppurativa Treatment?
For effective treatment, early diagnosis of hidradenitis suppurativa is key. Individuals should see a dermatologist if their condition is painful, scars, flares often, does not improve, returns within weeks of treatment, is unresponsive to topical therapy, or appears in several areas of the body.
Diagnosing Hidradenitis Suppurativa
Diagnosing hidradenitis suppurativa is primarily based on the clinical presentation of the disease. A dermatologist will conduct a physical examination and ask about your medical history, family history, and the hidradenitis suppurativa symptoms you’ve experienced. No specific blood tests confirm HS, but your provider may perform lab work to rule out infections or underlying disorders and assess disease severity.
In some cases, biopsies may be done to exclude other skin diseases, such as squamous cell carcinoma, or to assess chronic changes in affected skin. Accurate diagnosis is essential for proper systemic medical management, including topical treatment, biologic therapy, and surgical management, as well as for evaluating candidacy for clinical trials or emerging treatments.
Hidradenitis Suppurativa Treatments
There are a variety of treatment options available, which help to control symptoms and prevent complications. These include:
Antibiotic washes/creams: Mild hidradenitis suppurativa may be managed with topical antibacterial cleansers, lotion, and gels that fight infections.
Steroid Injections: A mainstay in the treatment of acute lesions is intralesional Kenalog.
Oral Antibiotics: Minocycline, doxycycline, rifampin, clindamycin, Bactrim, and quinolones are all used to treat moderate-severe hidradenitis suppurativa.
Hormonal drugs: Oral contraceptives, spironolactone, finasteride are sometimes used for chronic disease.
Biologic agents: Humira (adalimumab) subcutaneous injection may be used for moderate to severe disease in patients 12 and older. Other biologics used in our practice include IL-12/23 inhibitors, infliximab, and IL-17 inhibitors.
Anti-inflammatory drugs: Zinc, dapsone, acitretin/isotretinoin, metformin, prednisone, and methotrexate are less frequently used for recalcitrant disease.
Uncovering tunnels: Also known as unroofing, this involves removing tissues to expose the tunnels beneath the skin.
Punch debridement: Also called limited unroofing, this may be used to remove a single inflamed nodule.
Surgical removal: For individuals with persistent or severe symptoms, surgical removal may be an option. Individual lesions can be treated with Incision and Drainage or Simple Excision. In more extensive disease, all of the affected skin is removed, and a skin graft may be needed to close the wound. It is important to understand that sores may still occur in other areas of the body after surgery.
What to Expect During Hidradenitis Suppurativa Treatment?
Managing hidradenitis suppurativa involves a combination of complementary and procedural management approaches that are customized to the severity of your disease and your overall health. During treatment, your dermatologist will develop an individualized treatment plan. It’s important to avoid factors that irritate skin, such as tight clothing or aggressive shaving, and to maintain a gentle skincare routine. Treatment may involve managing chronic pain, controlling excessive sweating, and addressing mental health challenges related to living with HS.
Mild cases of hidradenitis suppurativa may also be managed with self-care measures. The following may help to relieve discomfort, prevent outbreaks, or speed up healing:
- Follow a daily skincare routine using a gentle non-soap cleanser or recommended benzoyl peroxide or Hibiclens wash. Avoid using washcloths or loofahs on affected areas
- Avoid wearing tight clothing and irritating products such as detergents with perfumes and dyes
- Avoid injuring the skin, including squeezing pimples and aggressive shaving of affected areas
- Avoid tobacco products, which can worsen symptoms
- Proper nutrition and weight loss if obese
What to Expect After Hidradenitis Suppurativa Treatment
Hidradenitis suppurativa treatment is meant to improve symptoms and help manage the condition. The length of your treatment and/or downtime will depend on the severity of your condition and your symptoms. Be sure to follow your dermatologist’s specific instructions on how to care for your skin post-treatment. Please do not hesitate to contact our office regarding treatment or post-treatment questions.
Schedule a Consultation
To schedule your hidradenitis suppurativa consultation today, contact HMGS Dermatology. Our skilled team of dermatologists and dermatology specialists is here to help you improve your skin and overall health.
Get Started With A Visit!
Fill out the form below and we will reach out to you shortly to schedule an appointment.
